Home > Blog
BLOG
Bone on Bone?? Or is it?
The Doctor Says I’m “Bone On Bone” !!
Time for total knee replacement… or is it?
There seems to be a discrepancy between real/actual knee joint health or status and the prevalence of patients reporting recommendations from medical professionals that their knee is “bone-on-bone” and recommends that the joint be replaced.
Regenerative medicine offers doctors an opportunity to provide pain relief for their patients without drastic surgical procedures such as a total knee replacement. It is important to understand that the proper application of a bio-cellular or regenerative medicine product does not remodel cartilage. However, if the cartilage interface (which has very little vascularity) remains intact, then we can initiate the repair mechanism by specifically targeting the peri-articular or supportive structures of the knee as well as the cartilage lined articular surfaces. This method can be of great benefit and circumvent a knee replacement. Furthermore, the chondrogenic properties of the infra-patellar fat pad should also be considered in regenerative medicine knee protocols.
The use of musculoskeletal (MSK) ultrasound is capable of clearly identifying whether or not a patient truly exhibits “bone-on-bone” by showing what is typically known as the “osteochondral” line. This is the interface between the cortical bone and the hyaline cartilage.
The cartilage interface, or lining, is one of the criteria for a joint to be considered a synovial joint. The other two criteria are a synovial membrane, and a joint capsule. The discrepancy of medical professionals incorrectly diagnosing knees as “bone-on-bone” may be clearly remedied with the employment of standard MSK ultrasound images which clearly demonstrate cartilage interfaces.
The images below were recently obtained from a patient who had been advised to have bilateral hip and knee replacements. Upon the use of MSK sonography, we were able to see that this diagnosis was not correct!
Image number one: the short axis view (perpendicular to the shaft of the femur) of the distal femur. Also known as the femoral trochlea. The bright/hyperechoic line is the cortical bone. The black/anechoic interface adjacent to the bone is the hyaline cartilage.
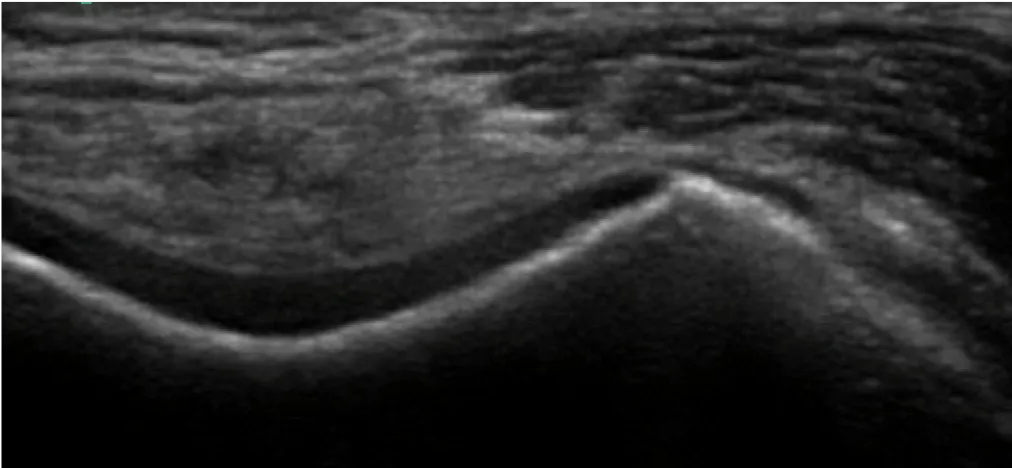
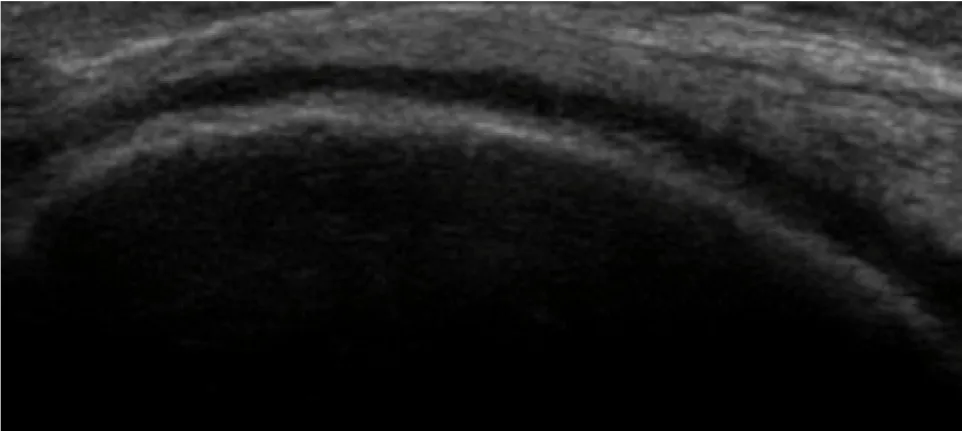
Image number two: the long axis view (parallel with the shaft of the femur) of the lateral femoral condyle. Again, the bright/hyperechoic line is the cortical bone of the condyle. Adjacent to the bone is the black/anechoic hyaline cartilage.
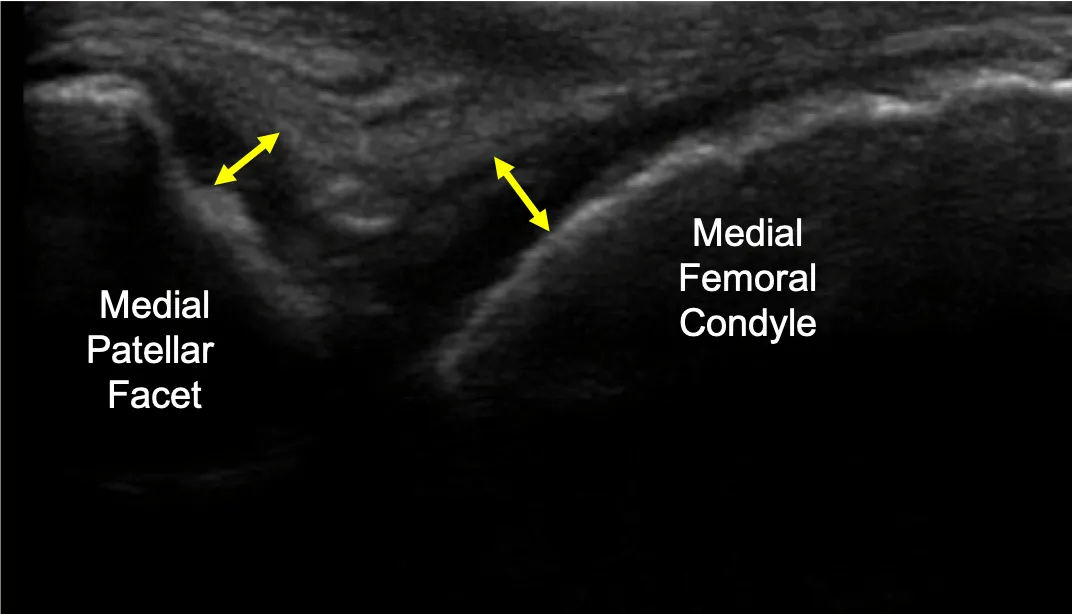
Image number three: is the short axis view (perpendicular to the shaft of the femur. The left side bone is the medial patella. The right side bone is the medial femur.) The yellow double-sided arrow indicates the thickness of the hyaline cartilage on the medial patellar facet.
It is not at all uncommon that I encounter nearly normal cartilage/articular surfaces in a diagnostic ultrasound exam of the knee with patients who have been advised to have total knee replacement. Developing and employing the “comprehensive AND targeted” treatment plan combined with a true high quality bio-cellular product is a viable and healthy alternative to joint replacement. Furthermore, patients who have been treated with regenerative therapy and still have joint replacement seem to have less post-surgical pain or apparent “failed outcomes”. All knee pain is not entirely generated from the degenerative joint space.


